Adrenal fatigue
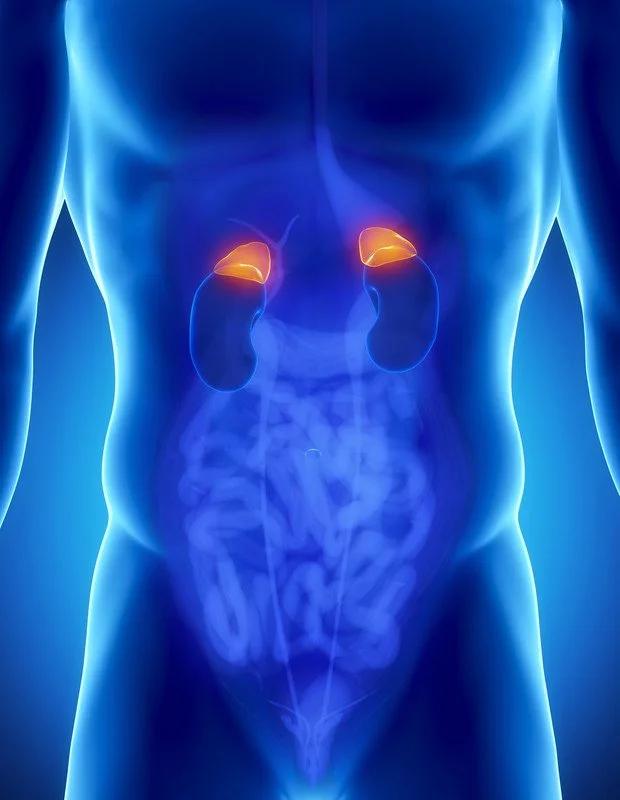
Your adrenal glands are each no bigger than a walnut and weigh less than a grape, yet are responsible for one of the most important functions in your body: managing your stress, both physical stress and emotional stress. The adrenals are the body's hormonal powerhouse. Two little glands that sit on top of your kidneys, they're the linchpin of a feedback loop coordinating nearly every hormone in your body.
When your adrenal glands are overtaxed, a condition known as adrenal fatigue or adrenal exhaustion sets in, which in turn can set a cascade of disease processes into motion. One tell-tale sign of adrenal burnout is feeling chronically fatigued. Another symptom that someone might experience it’s what called “tired but wired”, which means that even if you feel physically tired, you cannot fall asleep and you cannot function normal and have the undefined feeling that something is wrong.
It's estimated that up to 80 percent of adults experience adrenal fatigue during their lifetimes, yet it remains one of the most under-diagnosed illnesses in Canada.
The basis of adrenal fatigue or burnout is stress (or more correctly distress), which over time can tax your adrenal glands to the point of causing other health problems, such as:
Fatigue
Weight gain
Sleep disorders
Depression
The precipitating event for most people is a period of intense emotional stress. Based on my experience, approximately 95 percent of the patients report having experienced major emotional stress (life changing events) around the time their health began to falter.
There are three stages of adrenal fatigue. Each one is associated with a different type of cortisol imbalance, and typically people progress from stage 1 to stage 3 sequentially over time.
Stage 1: Wired and tired
This stage is characterized by high cortisol levels, especially at night, leading to insomnia, insulin resistance and abdominal weight gain. People often feel energized but in an edgy "wired" way.
Stage 2: Stressed and tired
In this stage, many people wake up early in the morning (often around 3am) and are unable to fall back asleep. Later in the day some stressor kicks in, and they feel more awake. Their cortisol peaks early, flattens out, but often has midday or early evening rise.
Stage 3: Burnout
This stage is characterized by exhaustion regardless of hours slept, a flat cortisol curve, and in some cases low DHEA and thyroid hormone levels.
For this condition our clinic will test your adrenal glands to better understand if this the cause of your problems. It will be followed by a Treatment Plan that will involve some adaptogenic plants, an adrenal nutraceutical formula, a change in diet to cool the inflammation ( a test to identify the foods you are sensitive too will also be suggested) and better hydration and rest.
LONELINESS and your health
There are more and more studies raising alarms about the impact of being lonely on our health. And the conclusions of those studies really shocked me so I decided to summarize and share this research in this blog.
But first of all, how did they define loneliness?
Loneliness is the cognitive discomfort or uneasiness of being or perceiving oneself to be alone, according to the American Psychological Association. It’s the emotional distress we feel when our inherent needs for intimacy (not necessarily sexual in nature) and connection aren’t met.
Loneliness causes people to feel empty, alone, and unwanted. People who are lonely often crave human contact, but their state of mind makes it more difficult to form connections with others.
It can bubble up as either an objective or subjective state. You could be objectively alone and crave companionship, or you could be in a crowded room and still feel alone in the world (the feeling of being alone). How many of us can say they did not feel this way at one point in their lives?...
Loneliness vs. Solitude
While research clearly shows that loneliness and isolation are bad for both mental and physical health, being alone is not the same as being lonely. In fact, solitude actually has a number of important mental health benefits, including allowing people to better focus and recharge.
Loneliness is marked by feelings of isolation despite wanting social connections. It is often perceived as an involuntary separation, rejection, or abandonment by other people.
Solitude, on the other hand, is voluntary. People who enjoy spending time by themselves continue to maintain positive social relationships that they can return to when they crave connection. They still spend time with others, but these interactions are balanced with periods of time alone.
So, this is what it was discovered studying loneliness:
1. Loneliness May Lead to Poor Health Habits
Evidence suggests people who feel lonelier may engage in more unhealthy behaviors compared with people who feel more socially connected. Research suggests single or widowed seniors eat fewer vegetables and fruits than their peers who are married or cohabitating. Other research found that people who are lonely were significantly less likely to exercise than people who felt less lonely.
2. Loneliness May Interfere with Sleep
Loneliness has been linked to insufficient sleep among older adults. Loneliness has also been linked to fragmented sleep, or more disrupted sleep. Researchers have suggested that we need to feel secure in our surroundings for a genuinely restful night’s sleep.
3. Loneliness May Increase Risk of Depression
Loneliness is a major risk factor for developing depression, with many symptoms overlapping (like experiencing feelings of pain and helplessness). In a study published in January 2021 in The Lancet Psychiatry, researchers concluded that loneliness increases the risk of depression, but that depression does not necessarily increase loneliness.
4. Loneliness May Trigger Chronic Inflammation
Inflammation is part of how our immune systems kick into action to protect us against harm or disease, or heal. Chronic inflammation is this process gone awry. The body continues to send distress signals even though there’s no injury or danger. This type of chronic inflammation causes chronic health problems, like heart disease, type 2 diabetes, rheumatoid arthritis, and cancer.
5. Chronic Loneliness Increases Dementia Risk
Adults who report greater feelings of loneliness are at a 40 percent increased risk of developing dementia and other cognitive impairments. Study participants were 50 and older. They completed surveys to measure loneliness and completed cognitive tests every two years over the course of a decade. The doctors say that people who were lonely had risk factors for diabetes, hypertension, depression, and other concerns, but even after adjusting for those shared risks, loneliness still predicted increased risk of dementia. There’s something about connecting with other people, having a reason to get up in the morning to engage with the world that protects the brain. It’s about keeping the brain active and, on its toes.
6. Loneliness Is Bad for Your Heart
Loneliness has been tied to a 29 percent increased risk of heart attack and a 32 percent increased risk of having a stroke, according to a meta-analysis published in April 2016 in the journal Heart. Previous research has also suggested that loneliness increases blood pressure.
7. Loneliness May Shorten Your Life
Ultimately, loneliness takes a grave toll on our health, with research suggesting that both living alone and feeling subjective loneliness increases risk of premature death by 29 and 26 percent. These findings stem from a meta-analysis that involved over 3.4 million participants, which was led by Holt-Lunstad and published in March 2015.
So, to summarize all these points, the conclusion of the authors all the majorities of these studies was this:
Loneliness can leave people feeling isolated and disconnected from others. It is a complex state of mind that can be caused by life changes, mental health conditions, poor self-esteem, and personality traits. Loneliness can also have serious health consequences including decreased mental wellness and physical problems.
Tips to Prevent and Overcome Loneliness
Loneliness can be overcome. It does require a conscious effort to make a change. In the long run, making a change can make you happier, healthier, and enable you to impact others around you in a positive way.
Here are some ways to prevent loneliness:
Consider community service or another activity that you enjoy. These situations present great opportunities to meet people and cultivate new friendships and social interactions.
Expect the best. Try to stay positive. Lonely people often expect rejection, so instead, try focusing on positive thoughts and attitudes in your social relationships.
Focus on developing quality relationships. Seek people who share similar attitudes, interests, and values with you. Experts believe that it is not the quantity of social interaction that combats loneliness, but the quality.
Recognize that loneliness is a sign that something needs to change. Don't expect things to change overnight, but you can start taking steps that will help relieve your feelings of loneliness and build connections that support your well-being.
Understand the effects of loneliness on your life. There are physical and mental repercussions to loneliness. If you recognize some of these symptoms affecting how you feel, make a conscious effort to combat them.
Join a group or start your own. For example, you might try creating a group where people from your area with similar interests can get together. You might also consider taking a class at a community college, joining a book club, or taking an exercise class.
Strengthen a current relationship. Building new connections is important, but improving your existing relationships can also be a great way to combat loneliness. Try calling a friend or family member you have spoken to in a while.
Talk to someone you can trust. Reaching out to someone in your life to talk about what you are feeling is important. This can be someone you know such as a family member, but you might also consider talking to your doctor or a therapist.
Berberine: An Ancient Compound with Modern Potential
Berberine is a naturally occurring bioactive compound that has attracted growing attention in recent years for its potential health benefits. Though it may sound like a newly discovered supplement trend, berberine has actually been used in traditional medicine systems for thousands of years.
What Is Berberine?
Berberine is an alkaloid found in several plants, including:
Berberis vulgaris (barberry)
Coptis chinensis (goldthread)
Hydrastis canadensis (goldenseal)
Berberis aquifolium (Oregon grape)
It is responsible for the bright yellow color of these plants’ roots and bark. Chemically, berberine belongs to a group of compounds known as isoquinoline alkaloids.
A Brief History of Berberine
Berberine-rich plants have been used for over 3,000 years in traditional systems of medicine.
Traditional Chinese Medicine
In Traditional Chinese Medicine (TCM), berberine-containing herbs like Coptis chinensis (Huang Lian) were prescribed to treat gastrointestinal infections, diarrhea, and inflammatory conditions. The compound was valued for its antimicrobial and "heat-clearing" properties.
Ayurvedic Medicine
In Ayurveda, barberry and related plants were used for digestive health, skin disorders, and metabolic imbalances.
Western Herbal Medicine
In Europe and North America, goldenseal and barberry were popular in 18th–19th century herbal practices, particularly for digestive complaints and infections before the antibiotic era.
How Berberine Works in the Body
Modern research has revealed that berberine acts on multiple biological pathways. One of its most studied mechanisms is its ability to activate an enzyme called AMP-activated protein kinase (AMPK), sometimes referred to as the body's "metabolic master switch."
By influencing AMPK and other pathways, berberine can affect:
Blood sugar regulation
Lipid (cholesterol and triglyceride) metabolism
Inflammatory responses
Gut microbiota balance
Common Uses of Berberine
1. Blood Sugar Support
One of the most researched uses of berberine is for type 2 diabetes and insulin resistance. Studies suggest it may help:
Lower fasting blood glucose
Improve insulin sensitivity
Reduce HbA1c levels
Some research has even compared its glucose-lowering effects to pharmaceutical medications, although it should not replace prescribed treatments without medical supervision.
2. Cholesterol and Heart Health
Berberine has been shown in several studies to help reduce:
LDL ("bad") cholesterol
Total cholesterol
Triglycerides
This makes it of interest for individuals with metabolic syndrome or cardiovascular risk factors.
3. Weight Management
Because of its influence on insulin and metabolism, berberine may assist in modest weight loss, particularly in individuals with insulin resistance. However, it is not a “magic pill” and works best alongside diet and exercise.
4. Gut Health and Antimicrobial Effects
Historically used for diarrhea and infections, berberine demonstrates antimicrobial activity against certain bacteria, fungi, and parasites. It may also help modulate the gut microbiome, although research is still developing in this area.
5. Polycystic Ovary Syndrome (PCOS)
Some research suggests berberine may improve insulin sensitivity and hormonal balance in women with PCOS, potentially supporting ovulation and metabolic health.
Safety and Side Effects
Berberine is generally considered safe for short-term use at recommended doses (commonly 500 mg two to three times daily), but it can cause side effects such as:
Digestive discomfort
Constipation or diarrhea
Low blood sugar (especially if combined with diabetes medications)
It should not be used during pregnancy or breastfeeding, and individuals taking prescription medications—especially for diabetes, blood pressure, or blood thinning—should consult a healthcare professional before use.
Modern Popularity
Today, berberine is widely available as a dietary supplement and has become popular in metabolic health communities. Interest has surged as people seek natural alternatives or complements to conventional treatments for diabetes and high cholesterol.
However, while promising, berberine is not a replacement for medical care. Its benefits are best viewed as complementary and should be discussed with a qualified healthcare provider.
Final Thoughts
Berberine is a fascinating example of how traditional herbal medicine and modern science can intersect. From ancient roots in Traditional Chinese Medicine and Ayurveda to contemporary research on metabolism and cardiovascular health, this yellow plant compound continues to generate interest.
As research evolves, berberine may further establish its place as a valuable tool in metabolic and digestive health—bridging thousands of years of tradition with modern biomedical understanding.
Blood – sacred fluid or commodity?
The history of blood in medicine and its symbolic meaning is as old as medicine itself.
Human beings, from ancient times, have viewed blood as miraculous, sacred, have been terrified of it, killed because of the “purity” or “impurity” of it and have died rather than betray it.
Blood is the ultimate symbol of life – a sacred fluid associated with birth, nobility, purity, fortitude, fertility and death. The ideas of monarchy and royalty rest upon the (outdated) notion of “blue blood” or pure blood that some members of our society acquire by simply being born from “noble” ancestors.
As a side note, a popular theory is that the phrase “blue blood” describes a condition caused by a rare genetic defect that is carried by the royal families of Europe due to their habit of only marrying from the same breeding pool, thus leading to a blood condition called hemophilia. In reality, the actual origin of the term “blue blood” comes from Spanish and it used to describe that when conquering lands held by Moors, the Spanish nobility displayed the fact that they had very white (never labored) untanned skin, though which blue veins were easily seen, in contrast with the darker skinned Moors.
All major cultures have used and treated blood in ways that reflect its symbolic importance. The Egyptians were mystified of blood and offered wine as “blood of the gods” for rituals; the Nile waters were turned to blood in the Ten Plagues of Egypt; the Egyptians bathed in blood to regain powers lost through illness or injury. The Mayans viewed blood as the supreme nourishment for their deities and the most important rituals culminated with a blood (human) sacrifice, either by decapitation or by heart removal.
Blood also plays a central role in the Christian sacramental traditions, where it is transformed into wine and consumed as the essence of life, the very presence of the “living God”, in the real belief that is the real presence of Christ in the Eucharist.
The science of blood took a major leap forward with the discovery of, by an English physician named William Harvey, the actual circulation of blood in humans, clarifying the role of the heart, lungs, arteries and veins in the circulatory system in a pamphlet called De Moto Cordis. It was 1628. Before this, it was presumed that the liver was the organ responsible for the “spontaneous” creation of blood from ingested food, a theory that lasted more than 1,000 years due to the crushing influence of Galen in this matter and in medicine in general.
The history of the blood as commodity begins with its value in saving lives through transfusion. According to some historians, the first attempt to transfuse blood from one human to another took place more than 500 years ago, when a dying Pope Innocent III received blood from 3 healthy boys with a disastrous results: the boys died, the Pope died and the physician fled the country!
Fast forward 500 years later, the technology has come to age. Countless lives are saved by transfusions all over the world. The science has started to de-mystify the blood and use it as a new commodity, with a market that started to come alive after the WWII. The years of 1950’s to 70’s were a boom in this market with blood being sold in USA at an ever growing pace. Then the ethical and moral issues started to become more prevalent and the desire to protect against the exploitations of those selling blood (usually poor, from low-income class). The open sale of blood created one of most bitter controversies over the ethics of establishing a commercial market for human body materials.
The boom in the increase worldwide sale of blood prompted various international agencies to act, encouraging governments and people alike for nonpaid blood donations as a compromise to the problem. Was blood a “gift”, retaining some of its symbolic sacredness, to be donated by and to a community as an act of social benevolence? Or it was a new commodity, a product, like a car, that could be advertised and sold like any other commodity?
The “gift concept” of blood donation and the blood volunteerism belief slowly advanced over the next two decades (70’s to 90’s) and finally triumphed in the USA, when an sustained campaign by the numerous agencies have managed to change the mindset from blood as commodity to blood donation in order to express compassion for their fellow men and women and to show devotion to their community.
This was a long journey for blood. From the magical, sacramental definitions of antiquity to the market definition of today. Blood and blood products (plasma, antibodies, clotting factors) are still being sold and bought around the world as a growing part of the pharmaceutical industry, becoming over the last 15 years a major medical commodity.
The debate over the paid versus nonpaid blood donations is still on.
Can a vitamin be a drug?
Sometimes patients are confused about this topic: aren’t the supplements (vitamin, minerals, fatty acids etc) drugs too? Don’t they “treat” diseases too? What’s the difference between them?
Let’s start with the definition of a drug first.
According to Health Canada, drugs include both prescription and non-prescription pharmaceuticals; biologically-derived products such as vaccines, blood derived products, and products produced through biotechnology; tissues and organs; disinfectants; and radio-pharmaceuticals. According to the Food and Drug Act, a drug includes any substance or mixture of substances manufactured, sold or represented for use in:
a. the diagnosis, treatment, mitigation or prevention of a disease, disorder, abnormal physical state, or the symptoms thereof in man or animal
b. restoring, correcting or modifying organic functions in man or animal, or
c. disinfection in premises in which food is manufactured, prepared or kept
Natural health products, such as vitamin and mineral supplements and herbal products for which therapeutic claims are made are also considered drugs at the level of the Food and Drugs Act; however, these products are regulated as natural health products under the Natural Health Products Regulations and not as drugs under the Food and Drug Regulations. They are seen as a sub-set of drugs now.
Another important theoretical distinction in the eyes of the authorities is this:
• Drugs are considered unsafe until proven safe
• Dietary supplements are considered safe until proven unsafe
Based on this conceptual difference, FDA and Health Canada consider new drugs to be unsafe until they are proven safe through clinical trials. And they must approve any new drug before it can be legally sold in the US or Canada. Clinical trials are studies done under well-controlled conditions on human volunteers. They are expensive. These tests must be done on all drugs – even those that are sold over the counter (without a prescription). The Health Canada approval process requires that the drug be proven in a series of clinical trials. These studies must show “substantial evidence” that the drug is both safe and effective for each of its intended uses. This level of scrutiny does not apply to natural health products. Manufacturers of supplements are not required to test new ingredients or supplements in clinical trials.
Under the Natural Health Products Regulations in Canada, which came into effect on January 1, 2004, natural health products (NHPs) are defined as:
• Vitamins and minerals
• Herbal remedies
• Homeopathic medicines
• Traditional medicines such as traditional Chinese medicines
• Probiotics
• Other products like amino acids and essential fatty acids
Vitamins and Minerals
Natural Health Products must be safe to use as over-the-counter products and not need a prescription to be sold. Vitamins and minerals are regulated as a sub-set of drugs because they are considered to be natural health products.
A quick search in the Drug Product Database for vitamins, mineral and other so perceived “natural products” will reveal this: vitamin A, D, Folic acid (vit.B9), vit.K1, vit.K2 all have this duality – they are dietary supplements that become drugs at certain dosages specified in the law.
Vitamin A, for example, requires a prescription when a practitioner recommends that a patient take more than 10,000 international units (IU) per dose or in the total daily intake. Similarly, vitamin D becomes a drug when taken at more than 1,000 IUs/day; vitamins K1 and K2 require a prescription at more than 0.120 mg per day.
Folic acid (vit.B9) also “behaves” like a drug when used “in oral dosage form containing more than 1.0 milligram of folic acid per dosage form or, where the largest recommended daily dosage shown on the label would, if consumed by a person, result in the daily intake by that person of more than 1.0 milligram of folic acid”.
Why is this important? For naturopaths who commonly incorporate recommendations for supplements and vitamins as part of their practice, this is extremely important. In order to do so at the levels noted above (where the vitamin becomes a drug), a naturopath must first have successfully completed the Ontario Therapeutic Prescribing course and examination. It is fairly common for naturopaths to recommend high dose vitamins to patients; however, naturopaths who recommend patients take vitamins at levels that are above the limits and who have not completed the necessary course and exam will have breached the regulation and are subject to prosecution by the College for professional misconduct.
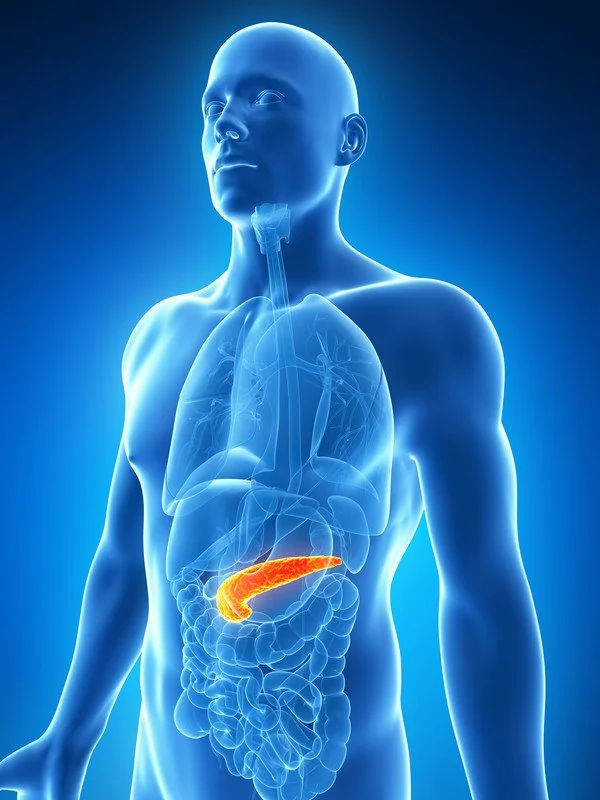
Alcohol and the Pancreas
Pancreas in the human body
Pancreatic cancer is one of the deadliest forms of cancer. Each year, approximately 5.500 people are diagnosed with pancreatic cancer in Canada and more than 4,800 will die from it (87%). The disease is often diagnosed at an advanced stage, and improved approaches to early detection and treatment are very important for doctors and researchers.
It has long been known that heavy drinking can damages the pancreas and that excessive alcohol consumption can contribute to pancreatitis, an inflammation of the pancreas characterized by severe abdominal pain, nausea, fever, sweating and vomiting.
How much is too much?
People who consumed three or more alcohol beverages per day were more likely to die of pancreatic cancer than non-drinkers. Among never-smokers, heavy drinking increased the risk of pancreatic death by 36%. Among those who had ever smoked, heavy drinking increased the risk of pancreatic cancer death by 16%.
Liquor was more strongly linked with pancreatic cancer death than beer or wine. Why? Wine and beer both contain polyphenols, which are antioxidants that neutralize harmful oxidation and alcohol damages the pancreas by inducing oxidative stress.
How the alcohol can affect the pancreas? I have been thinking of this lately because I couldn’t see the association.
At the first glance it seems like a long stretch but science has (mostly) figured it out.
The pancreas is flat gland that sits behind the stomach. It’s responsible for producing the hormones insulin and glucagon (endocrine function) as well as enzymes (exocrine function) that help to digest food. The pancreas is particularly sensitive to alcohol.
One theory says this: Alcohol is partially metabolized in the pancreas and some of the early metabolites of alcohol (acetaldehyde) can be toxic to the cells. They can lead to changes in pathways that are important to cancer like the tilting the balance toward the pathway of chronic inflammation. And this that leads to scarring of the pancreatic tissue. Scarring means inflammation, chronic inflammation means cancer.
Another theory: alcohol damages the endocrine cells and interferes with the metabolic processes of the pancreas. Instead of sending the digestive enzymes to the small intestine to process the food, the pancreas gets confused and secretes the digestive juices internally. The problem is that the pancreas isn’t designed to receive these juices, which are harmful to the pancreas. As a result, prolonged alcohol abuse can lead to an inflammation known as pancreatitis.
One last theory suggest that the chemical reactions between the breakdown of alcohol and pancreatic fluids form small plugs that clog up the pancreas and obstruct the flow of pancreatic fluids. When this happens, the enzymes are activated inside the pancreas. The pancreas digests itself. The enzymes attack and damage the pancreas causing scar tissue to form. As the scar tissue develops the pancreas is slowly destroyed, leading to pancreatitis and, in time, to pancreatic cancer.
What’s been harder for scientists to prove, however, was that alcohol increases the risk of pancreatic cancer largely because most studies have been too small in the past. Most of the quality studies are observational and prove only the association between alcohol and pancreatic cancer not the causality.
In conclusion: stick to beer and wine, no more than one glass a day and you will live wise and happy!
AI in Medicine
I have been wondering these days what is the status of the applications of AI in medicine…is it how many are predicting that the AI will carve out a hole in medicine? Will the doctors be replaced by machine anytime soon?
Let’s see what we can find out.
I think it is safe to say that there are top 4 applications of AI in medicine today:
1. Diagnose diseases
Correctly diagnosing diseases takes years of medical training. This is a science and an art, at the same time. Even then, diagnostics is often an laborious, time-consuming process. In many fields, the demand for experts far exceeds the available supply. This puts doctors under strain and often delays life-saving patient diagnostics.
Machine Learning – particularly Deep Learning algorithms – have recently made huge advances in automatically diagnosing diseases, making diagnostics cheaper and more accessible.
How machines learn to diagnose
Machine Learning algorithms can learn to see patterns similarly to the way doctors see them. A key difference is that algorithms need a lot of concrete examples – many thousands – in order to learn. And these examples need to be neatly digitized – machines can’t read between the lines in textbooks, like humans do.
So, Machine Learning is particularly helpful in areas where the diagnostic information a doctor examines is already digitized.
Good examples?
Detecting lung cancer or strokes based on CT scans
Assessing the risk of sudden cardiac death or other heart diseases based on electrocardiograms and cardiac MRI images
Classifying skin lesions in skin images
Finding indicators of diabetic retinopathy in eye images
Since there is plenty of good data available in these cases, algorithms are becoming just as good at diagnostics as the experts. The difference is: the algorithm can draw conclusions in a fraction of a second, and it can be reproduced inexpensively all over the world. Soon everyone, everywhere could have access to the same quality of top expert in radiology diagnostics, and for a low price.
More advanced AI diagnostics are coming soon
The application of Machine Learning in diagnostics is just beginning – more ambitious systems involve the combination of multiple data sources (CT, MRI, genomics and proteomics, patient data, and even handwritten files) in assessing a disease or its progression. But this will take time.
AI won’t replace doctors anytime soon
It’s unlikely that AI will replace doctors outright here. Instead, AI systems will be used to highlight potentially malignant lesions or dangerous cardiac patterns for the expert – allowing the doctor to focus on the interpretation of those signals. The machine will give the doctors choices. The doctor will take the best course of action then.
2. Develop drugs faster
Developing drugs is a notoriously long and expensive process. Many of the analytical processes involved in drug development can be made more efficient with Machine Learning. This has the potential to shave off years of work and hundreds of millions in investments.
AI has already been used successfully in all of the 4 main stages in drug development:
Stage 1: Identifying targets for intervention
Stage 2: Discovering drug candidates
Stage 3: Speeding up clinical trials
Stage 4: Finding Biomarkers for diagnosing the disease
Stage 1: Identify targets for intervention
The first step in drug development is understanding the biological origin of a disease (pathways) as well as its resistance mechanisms. Then you have to identify good targets (typically proteins) for treating the disease. The widespread availability of high-throughput techniques, such as short hairpin RNA (shRNA) screening and deep sequencing, has greatly increased the amount of data available for discovering viable target pathways. However, with traditional techniques, it’s still a challenge to integrate the high number and variety of data sources – and then find the relevant patterns.
Machine Learning algorithms can more easily analyse all the available data and can even learn to automatically identify good target proteins.
Stage 2: Discover drug candidates
Next, you need to find a compound that can interact with the identified target molecule in the desired way. This involves screening a large number – often many thousands or even millions – of potential compounds for their effect on the target (affinity), not to mention their off-target side-effects (toxicity). These compounds could be natural, synthetic, or bioengineered.
However, current software is often inaccurate and produces a lot of bad suggestions (false positives) – so it takes a very long time to narrow it down to the best drug candidates (known as leads).
Machine Learning algorithms can also help here: They can learn to predict the suitability of a molecule based on structural fingerprints and molecular descriptors. Then they blaze through millions of potential molecules and filter them all down to the best options – those that also have minimal side effects. This ends up saving a lot of time in drug design.
Stage 3: Speed up clinical trials
It’s hard to find suitable candidates for clinical trials. If you choose the wrong candidates, it will prolong the trial – costing a lot of time and resources.
Machine Learning can speed up the design of clinical trials by automatically identifying suitable candidates as well as ensuring the correct distribution for groups of trial participants. Algorithms can help identify patterns that separate good candidates from bad. They can also serve as an early warning system for a clinical trial that is not producing conclusive results – allowing the researchers to intervene earlier, and potentially saving the development of the drug.
Stage 4: Find Biomarkers for diagnosing the disease
You can only treat patients for a disease once you’re sure of your diagnosis. Some methods are very expensive and involve complicated lab equipment as well as expert knowledge – such as whole genome sequencing.
Biomarkers are molecules found in bodily fluids (typically human blood) that provide absolute certainty as to whether or not a patient has a disease. They make the process of diagnosing a disease secure and cheap.
You can also use them to pinpoint the progression of the disease – making it easier for doctors to choose the correct treatment and monitor whether the drug is working.
But discovering suitable Biomarkers for a particular disease is hard. It’s another expensive, time-consuming process that involves screening tens of thousands of potential molecule candidates.
AI can automate a large portion of the manual work and speed up the process. The algorithms classify molecules into good and bad candidates – which helps clinicians focus on analysing the best prospects.
Biomarkers can be used to identify:
The presence of a disease as early as possible - diagnostic biomarker
The risk of a patient developing the disease - risk biomarker
The likely progress of a disease - prognostic biomarker
Whether a patient will respond to a drug - predictive biomarker
3. Personalize treatment
Different patients respond to drugs and treatment schedules differently. So personalized treatment has enormous potential to increase patients’ lifespans. But it’s very hard to identify which factors should affect the choice of treatment.
Machine Learning can automate this complicated statistical work – and help discover which characteristics indicate that a patient will have a particular response to a particular treatment. So, the algorithm can predict a patient’s probable response to a particular treatment.
The system learns this by cross-referencing similar patients and comparing their treatments and outcomes. The resulting outcome predictions make it much easier for doctors to design the right treatment plan.
4. Improve gene editing
Clustered Regularly Interspaced Short Palindromic Repeats (CRISPR), specifically the CRISPR-Cas9 system for gene editing, is a big leap forward in our ability to edit DNA cost effectively – and precisely, like a surgeon.
This technique relies on short guide RNAs (sgRNA) to target and edit a specific location on the DNA. But the guide RNA can fit multiple DNA locations – and that can lead to unintended side effects (off-target effects). The careful selection of guide RNA with the least dangerous side effects is a major bottleneck in the application of the CRISPR system.
Machine Learning models have been proven to produce the best results when it comes to predicting the degree of both guide-target interactions and off-target effects for a given sgRNA. This can significantly speed up the development of guide RNA for every region of human DNA. This is the future of medicine, I personally think.
My conclusion: AI will impact the work of many people in the healthcare industry, but there’s no need to fear. Machines won’t be replacing healthcare providers anytime soon.
Redefine Success
It All Begins Here
Confidence doesn’t always arrive with a bold entrance. Sometimes, it builds quietly, step by step, as we show up for ourselves day after day. It grows when we choose to try, even when we’re unsure of the outcome. Every time you take action despite self-doubt, you reinforce the belief that you’re capable. Confidence isn’t about having all the answers — it’s about trusting that you can figure it out along the way.
The key to making things happen isn’t waiting for the perfect moment; it’s starting with what you have, where you are. Big goals can feel overwhelming when viewed all at once, but momentum builds through small, consistent action. Whether you’re working toward a personal milestone or a professional dream, progress comes from showing up — not perfectly, but persistently. Action creates clarity, and over time, those steps forward add up to something real.
You don’t need to be fearless to reach your goals, you just need to be willing. Willing to try, willing to learn, and willing to believe that you’re capable of more than you know. The road may not always be smooth, but growth rarely is. What matters most is that you keep going, keep learning, and keep believing in the version of yourself you’re becoming.
Small Steps Create Big Shifts
It All Begins Here
Confidence doesn’t always arrive with a bold entrance. Sometimes, it builds quietly, step by step, as we show up for ourselves day after day. It grows when we choose to try, even when we’re unsure of the outcome. Every time you take action despite self-doubt, you reinforce the belief that you’re capable. Confidence isn’t about having all the answers — it’s about trusting that you can figure it out along the way.
The key to making things happen isn’t waiting for the perfect moment; it’s starting with what you have, where you are. Big goals can feel overwhelming when viewed all at once, but momentum builds through small, consistent action. Whether you’re working toward a personal milestone or a professional dream, progress comes from showing up — not perfectly, but persistently. Action creates clarity, and over time, those steps forward add up to something real.
You don’t need to be fearless to reach your goals, you just need to be willing. Willing to try, willing to learn, and willing to believe that you’re capable of more than you know. The road may not always be smooth, but growth rarely is. What matters most is that you keep going, keep learning, and keep believing in the version of yourself you’re becoming.
Turn Intention Into Action
It All Begins Here
Confidence doesn’t always arrive with a bold entrance. Sometimes, it builds quietly, step by step, as we show up for ourselves day after day. It grows when we choose to try, even when we’re unsure of the outcome. Every time you take action despite self-doubt, you reinforce the belief that you’re capable. Confidence isn’t about having all the answers — it’s about trusting that you can figure it out along the way.
The key to making things happen isn’t waiting for the perfect moment; it’s starting with what you have, where you are. Big goals can feel overwhelming when viewed all at once, but momentum builds through small, consistent action. Whether you’re working toward a personal milestone or a professional dream, progress comes from showing up — not perfectly, but persistently. Action creates clarity, and over time, those steps forward add up to something real.
You don’t need to be fearless to reach your goals, you just need to be willing. Willing to try, willing to learn, and willing to believe that you’re capable of more than you know. The road may not always be smooth, but growth rarely is. What matters most is that you keep going, keep learning, and keep believing in the version of yourself you’re becoming.
Make Room for Growth
It All Begins Here
Confidence doesn’t always arrive with a bold entrance. Sometimes, it builds quietly, step by step, as we show up for ourselves day after day. It grows when we choose to try, even when we’re unsure of the outcome. Every time you take action despite self-doubt, you reinforce the belief that you’re capable. Confidence isn’t about having all the answers — it’s about trusting that you can figure it out along the way.
The key to making things happen isn’t waiting for the perfect moment; it’s starting with what you have, where you are. Big goals can feel overwhelming when viewed all at once, but momentum builds through small, consistent action. Whether you’re working toward a personal milestone or a professional dream, progress comes from showing up — not perfectly, but persistently. Action creates clarity, and over time, those steps forward add up to something real.
You don’t need to be fearless to reach your goals, you just need to be willing. Willing to try, willing to learn, and willing to believe that you’re capable of more than you know. The road may not always be smooth, but growth rarely is. What matters most is that you keep going, keep learning, and keep believing in the version of yourself you’re becoming.